Patients with various types of spinal cord injury and different neurological problems as stroke, multiple sclerosis and Parkinsonism can suffer from different urologic problems including urinary incontinence as a result of bladder and sphincteric dysfunction, recurrent urinary tract infection, urinary stone diseases, deterioration of kidney function and sexual dysfunction.
At West coast Urology, we have the most advance technology in evaluating the bladder and sphincetric function using VideoUrodynamic with pelvic floor motion. This will provide us with adequate information on how to manage the neurogenic bladder and the urinary problems that can result from it.
What is Neurogenic Bladder?
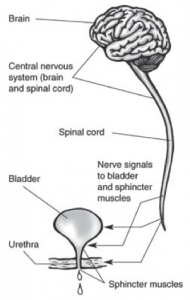
Neurogenic bladder is a bladder dysfunction resulting from improper functioning of the nerves, which carry messages between the brain and the bladder muscles to facilitate urination. Proper bladder function depends on these nerves to sense the fullness of the bladder and to retain or release urine.
Any condition that impairs bladder and sphincter afferent and efferent nerves can cause neurogenic bladder. Causes may involve the CNS (eg, stroke, spinal cord injury, meningomyelocele, amyotrophic lateral sclerosis), peripheral nerves (eg, diabetic, alcoholic, or vitamin B12 deficiency neuropathies; herniated disks; damage due to pelvic nerves as a result of extensive pelvic surgery), or both (eg, Parkinson disease, multiple sclerosis, syphilis).
In flaccid (hypotonic) neurogenic bladder, volume is large, pressure is low, and contractions are absent. It may result from peripheral nerve damage or spinal cord damage at the S2 to S4 level. After acute cord damage, initial flaccidity may be followed by long-term flaccidity or spasticity, or bladder function may improve after days, weeks, or months. Overflow incontinence is the primary symptom in patients with a flaccid bladder. Patients retain urine and have constant overflow dribbling. Men typically also have erectile dysfunction.
In spastic bladder, volume is typically normal or small, and involuntary contractions occur. It usually results from brain damage or spinal cord damage above T12. Precise symptoms vary by site and severity of the lesion. Bladder contraction and external urinary sphincter relaxation are typically uncoordinated (detrusor-sphincter dyssynergia). Patients with spastic bladder may have frequency, nocturia, and spastic paralysis with sensory deficits; most have intermittent bladder contractions causing urine leakage and, unless they lack sensation, urgency. In patients with detrusor-sphincter dyssynergia, sphincter spasm during voiding may prevent complete bladder emptying and can cause damage to the kidneys.
Mixed patterns (flaccid and spastic bladder) may be caused by many disorders, including syphilis, diabetes mellitus, brain or spinal cord tumors, stroke, ruptured intervertebral disk, and demyelinating or degenerative disorders (eg, multiple sclerosis, amyotrophic lateral sclerosis).
Complications of Neurogenic bladder:
High-pressure spastic bladders are more dangerous then low-pressure flaccid bladders.
Common complications include recurrent UTIs and urinary calculi. Hydronephrosis with vesicoureteral reflux may occur because the large urine volume puts pressure on the vesicoureteral junction, causing dysfunction with reflux and, in severe cases, nephropathy. Patients with high thoracic or cervical spinal cord lesions are at risk of autonomic dysreflexia (a life-threatening syndrome of malignant hypertension, bradycardia or tachycardia, headache, piloerection, and sweating due to unregulated sympathetic hyperactivity). This disorder may be triggered by acute bladder distention (due to urinary retention) or bowel distention (due to constipation or fecal impaction).
Evaluation of neurogenic bladder
The primary goal of evaluation is to determine, if this is a low-pressure flaccid or high-pressure spastic bladder. The latter carries a high risk of damaging the kidneys if not managed properly
Evaluation should include
- Renal ultrasonography
- VideoUrodynamic
- Cystoscopy
Treatment
The primary goals of treatment are
1-Achieve adequate and efficient drainage of the bladder
2-Maintain low-pressure bladder to avoid damage of the upper tract
3-Imporve incontinence.
This can be achieved using special bladder and pelvic floor rehabilitation programs, clean intermittent catheterization, different medications, Botox injection, Neuromodulation and various surgical procedures to improve bladder size and function as well as sphincter mechanisms