Male Prostate Health
What is the prostate?
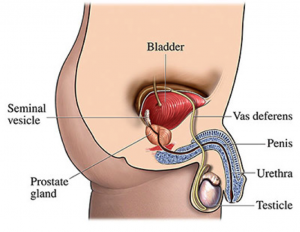
The prostate is part of the male reproductive system. It a walnut-sized gland located beneath the bladder and in front of the rectum in men. The prostate is surrounded by muscles and nerves. It surrounds the urine channel or the urethra (tube that carries the urine and semen out of the body). The prostate’s main job is to help make fluid for semen. This seminal fluid protects and energizes sperm as they travel to the female egg.
How to examine the prostate
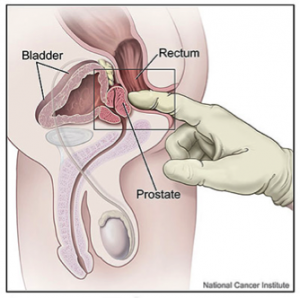
The only way to feel the prostate is through Digital rectal exam (DRE). This is done by putting a lubricated, gloved finger into your rectum. Pressure on the prostate can cause pain and urge to urinate. You might be asked to give a specimen of urine after prostate examination if infection is suspected.
Transrectal Ultrasound
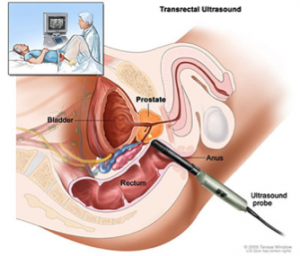
To get a closer look at the prostate gland, transrectal ultrasound can be used. Ultrasound machine uses sound waves bouncing off an organ to show a picture of the organ. To “see” the prostate, the ultrasound probe is placed in the rectum.
Three conditions can affect your prostate
A-Infection: Prostatitis
B- Benign enlargement of the prostate: BPH
C- Prostate cancer
A-Prostatitis
There are 3 common types of prostatitis:
- Acute (Sudden) Bacterial Prostatitis
- Chronic Bacterial Prostatitis
- Chronic non bacterial Prostatitis/Chronic Pelvic Pain Syndrome (CP/CPPS)
Acute Bacterial Prostatitis:
Acute prostatitis is a common, painful infection of the prostate that can occur in men of all ages.
The cause of most cases of acute prostatitis is bacterial infection. It is not always clear how bacteria can reach the prostate. Most likely, bacteria get into the prostate when infected urine flows backwards from the urethra. Certain factors can increase your risk including
- Obstruction of the lower urinary tract, i.e., the bladder and the urethra
- Presence of a catheter (a tube to drain bladder) or other instrument recently placed in your urethra
- Recent bladder infection
Bacterial prostatitis cannot be passed from one person to another during sex. So a sex partner can’t catch this infection.
Symptoms of acute prostatitis are usually sudden and painful. They include:
- Chills
- Fever
- Severe burning while urinating
- Difficult urinating
Diagnosis:
This includes digital rectal examination (DRE). When the prostate is massaged during the DRE, a fluid called expressed prostatic excretion (EPS) comes out of the penis. Urine and EPS are checked for signs of inflammation and infection.
We always like to check your prostate specific antigen (PSA) level. This is usually elevated in acute prostatitis.
Urine Flow Studies
You will be asked to urinate in a special machine that will measure the strength of your flow and determine if you are able to empty your bladder well. These tests will help to determine if there is any blockage caused by the prostate, urethra, or pelvic muscles.
Treatment includes antibiotics, anti-inflammatories and analgesics. It is difficult for antibiotics to reach the prostate, so you will need to continue taking antibiotics for at least 3-4 weeks even if your symptoms improve. Occasionally, You may be admitted to the hospital and given antibiotics through an IV (into your vein). If you have trouble urinating, you may need a catheter to drain your bladder.
Chronic Bacterial Prostatitis
This occurs if infection is not adequately treated during acute stage. Symptoms may recur over a long period of time.
These include:
- Burning feeling while urinating
- Need to urinate often (mainly during the night)
- Pain in the bladder, testicles, penis, and between the sex organs and anus
- Painful ejaculation
For chronic bacterial prostatitis, you’ll need to take antibiotics longer, most often for 4 to 12 weeks. About 3 in 4 of chronic bacterial prostatitis cases clear up with this treatment. Sometimes the symptoms return and antibiotics are needed again.
Chronic Prostatitis/Chronic Pelvic Pain Syndrome (CP/CPPS)
This condition is known as Chronic non-bacterial prostatitis , prostadynia or
chronic pelvic pain syndrome. This is the most common form of prostatitis, accounting for 90% of the cases. The condition is marked by pelvic, perineal and genital pain for long time. Patients usually have received many courses of antibiotics have no bacteria in their urine.
The exact etiology of CP/CPPS is not clear. Some believe that it may be caused by unusual organisms as chlamydia, mycoplasma (which may be passed during sex), or ureaplasma. Others, consider it as a reaction to an infection or injury that happened in the past with irritation of the surrounding nerves and pelvic floor muscles.
The condition can be confused with interstitial cystitis or painful bladder syndrome (a chronic inflammation of the bladder).
Patients with CP/CPPS usually complain for a long time of
- Pain in the pelvis, testicles, penis, and between the sex organs and anus
- Difficult urination
- Pain and discomfort with urination
- Trouble and pain with ejaculation
Treatment of CP/CPPS is very difficult and usually requires multimodalities including diet modification, behavior changes, medications to help relax the muscles around the prostate and the base of the bladder, anti-inflammatory drugs, pain medications, muscle relaxants.
Prostatic massages can help ease pressure by draining fluid from the prostate ducts while specialized physiotherapy and biofeedback may relax the nearby muscles.
Hot baths, hot water bottles, or heating pads may help ease pain. If sitting is painful, a donut pillow or inflatable cushion may help.
Occasionally, long-term antibiotics may be needed.
B- Benign prostatic enlargement and voiding dysfunction:
Benign Prostatic Hyperplasia, or “BPH,” is the non-cancerous (benign) enlargement of the prostate gland. The prostate starts to grow at puberty under the influence of the male hormone Testosterone. As the prostate gets bigger with age, it compresses the urethra. (the urinary channel that runs through the middle of the prostate and extends from the bladder to the penile urethra.) and obstruct the flow of the urine. When the prostate reaches a significant size, the patient starts to experience significant urinary symptoms known as LUTS. These include the need to urinate frequently especially at night, a weak urine flow, sudden urge to urinate (urgency), trouble staring and stopping your urine stream and sense of incomplete emptying of your bladder. These symptoms are bothersome, and can interfere with your quality of life.
To determine the severity of your symptoms, the American Urological Association has developed a questionnaire called the AUA symptom score.
Evaluation:
The initial evaluation for patients with BPH is Uroflowmetery to measure the force of the stream and post-void residual to assess the ability to empty your bladder. Many of the symptoms in patients with BPH are related to bladder dysfunction that developed as a result of enlargement and long-standing obstruction by the prostate. Dr. Aboseif strongly believes that all patients should have proper evaluation of their bladder function prior to any surgical therapy of the prostate, using video-urodynamic testing. Patients with poor bladder function will need special management of their bladder prior to any surgical intervention.
Medical Management of BPH
There are oral medications available by prescription for treating BPH. These include a group of drugs known as alpha blockers. These agents work by relaxing the muscles within the prostate, resulting in less pressure on the urethra and a more efficient flow of urine. This group include Cardura , Hytrin , Flowmax, Rapaflo, Uroxatral. One of the main side effects of these drugs include retrograde ejaculation, where the semen goes back to the bladder
Other medications treat prostate enlargement by blocking certain hormones related to testosterone. These oral medications include Proscar and Avodart; they may cause the prostate to gradually shrink, improving symptoms for some patients; but this shrinking or “downsizing” of the prostate may take from six to twelve months, and not all patients respond well to this treatment.
Recently, medications initially used to treat erectile dysfunction have been used successfully in patients with BPH. This includes Cialis and Viagra. They are given as a daily dose and can help patients with both ED and voiding problems with minimal side effects.
Surgical Treatment of BPH
Our center is experienced in different surgical approach for BPH. It is very important to determine the size of the prostate using transrectal ultrasound in-order to determine the safest approach that will give the best surgical outcome. Surgical options for enlarged prostate include: thermal therapy (microwave, TUNA), Green light laser, bipolar transurethral resection of the prostate (TURP) using the latest technology in electric current, and simple robotic prostatectomy. Most new surgical treatment of BPH will be done as an outpatient procedure.
Minimally invasive Thermal therapy for the prostate:
Transurethral needle ablation of the prostate (TUNA)
Transurethral microwave therapy of the prostate (TUMT)
Thermal therapy is a minimally invasive therapy for BPH. It relies upon the slow heating of prostate tissue with radiant heat such as that generated in microwave or radiofrequency therapy. With the application of heat, changes occur to the cells in these areas—over a period of days or weeks, they shrink. Both procedures are indicated for mild enlargement of the prostate. In cases where the prostate protrudes into the bladder, known as a large median lobe, only TUNA can be used.
- A- “TUNA” (transurethral needle ablation of the prostate) or Prostiva.
- This is an office procedure done under local anesthetic and some sedation. It uses low-level radiofrequency energy to destroy excess prostatic tissues without damaging the urethra or the surrounding tissues. It involves using a scope to pass a pair of fine needles through the lining of the prostatic urethra. Once the needles are in place, a radiofrequency signal passed through them to gently heat the region. The physician will likely treat several sites within your prostate. The procedure takes about 45 minutes. This shrinks the prostate tissue, causing the prostatic urethra to enlarge; the result is a higher and more efficient flow of urine. The maximum effect is usually seen in 4-6 weeks. Most patients are able to resume regular activity in 24-48 hours. A catheter is usually necessary following treatment for about 2-3 days. Side effects, which are usually minor and resolve without intervention during the healing period, include blood in the urine (hematuria) , discomfort or pain usually relieved using over- the –counter pain relievers, and urinary tract infection. Long-term complications (e.g., urinary incontinence, sexual dysfunction) are unusual and occur less often than following conventional procedure such as TURP
- B- “TUMT” Transurethral Microwave Therapy for the prostate or Prolieve
This is an in-office procedure done under local anesthetic and some sedation. A small catheter is inserted into the urethra. A small balloon that is also part of the catheter inflates within the section of the urethra close to the prostate. A special antenna inside the catheter transmits microwave energy to provide heat to the prostate. The heat reduces the prostate enlarged tissues. During the entire 45-minute procedure, water circulates inside the catheter through the urethra. As a safeguard, the Prolieve System’s computer monitors the temperature surrounding the treatment area by means of a rectal temperature monitor. If the temperature at the monitor reaches 42ºC (about 107º F), the system shuts off automatically.
Medication is often administered to reduce discomfort and help patients relax during the procedure. Many patients are able to read, watch television, or listen to music during treatment and some may experience the following:
- Bladder spasms
- Pressure in the rectum
- Sensation of needing to empty the bladder or have a bowel movement.
- Warm or burning sensation in the abdomen or penis
What Will Happen After TUNA or TUMT Procedure?
After the procedure is complete, you may be asked to remain in the office until you urinate. If you are not able to urinate after the procedure, your doctor may elect to insert a catheter to ensure your comfort.
Catheterization is required only as needed, and when required, the duration is usually a maximum of two days..
Upon arriving home, you should drink plenty of fluids. You should be able to return to most of your normal activities within 24 to 48 hours. There is minimal discomfort after the therapy. This can be relieved with over-the-counter pain medicines as needed.
You should relax and take it easy when you get home. You can expect optimal results in approximately six weeks; some patients may experience results sooner.
Possible side effects include obstruction, bleeding, blood in urine, pain/discomfort, urgency to urinate, increased frequency and urinary tract infection. Patients may also experience a minor burning sensation when urinating for one to two weeks following the treatment.
Laser Therapy for prostate:
Laser is widely used in different surgical procedures. The laser fibers deliver high power energy, which precisely cut and coagulates the tissue at the same time, causing minimal bleeding and damage to the surrounding structures.. There are several types of laser, the one most commonly used in prostate is called Green-Light laser. The laser fiber delivers very high energy, which quickly heats up the prostate tissue, causing it to vaporize. The process is continued until all of the enlarged prostate tissue has been removed. Normal urine flow is rapidly restored after the procedure and urinary symptoms are quickly relieved in most patients.
GreenLight laser combines the effectiveness of the “Gold standard” transurethral resection of the prostate (TURP) surgical procedure with less bleeding and fewer side effects.
GreenLight laser can be performed in outpatient center under general or spinal anasthetic. Typically, no overnight stay is needed. However, in some cases an overnight stay may be recommended when a patient travels long distance, or has other medical conditions to consider.
Bipolar TURP uses uses the latest technology in electric current. It is very effective in reliving the obstruction by removing the central portion of the prostate. It has advantages over traditional TURP, such as virtually eliminating “TUR Syndrome” related to systemic absorption of water irrigation, since this procedure is done using isotonic saline or glycine.